Sciatica has become one of the most commonly reported nerve-related pain conditions worldwide. More people today are complaining of sharp, burning pain that runs from the lower back through the buttocks and down the leg. While sciatica itself is not a new disease, its frequency and visibility appear to be rising, especially in urban and sedentary populations.
To understand this trend, we need to look at both medical causes and modern lifestyle changes.
1. What Exactly Is Sciatica?
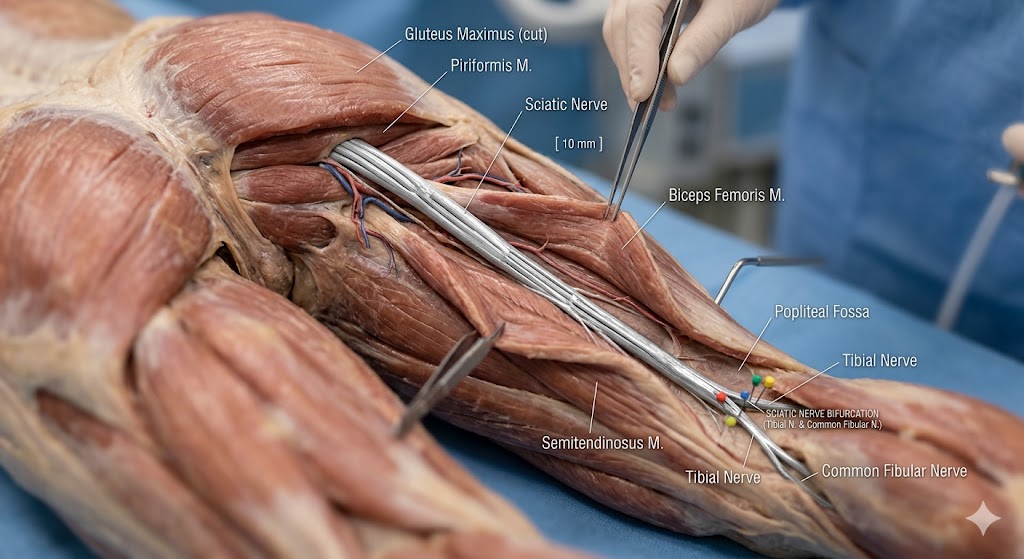
Sciatica is not a disease by itself, but a symptom of irritation or compression of the sciatic nerve—the longest nerve in the human body. It runs from the lower spine through the hips and down each leg.
When this nerve is irritated, it can cause:
- Sharp or burning pain in the lower back or leg
- Tingling or “pins and needles”
- Numbness
- Muscle weakness in the leg or foot
Most cases affect only one side of the body.
2. Medical Causes of Sciatica (The Core Problem)
In most cases, sciatica is caused by pressure on the nerve roots in the lower spine.
The most common underlying conditions include:
a) Herniated or Bulging Discs
This is the leading cause. A spinal disc pushes out and presses on the nerve roots.
b) Spinal Degeneration (Wear and Tear)
As we age, spinal joints and discs weaken, leading to nerve compression.
c) Spinal Stenosis
This is a narrowing of the spinal canal that squeezes nerves.
d) Bone Spurs (Arthritis-related growths)
Extra bone growth can press on nerve pathways.
e) Less common causes
- Injuries or trauma
- Pregnancy-related pressure
- Tumors (rare)
- Muscle-related nerve irritation (e.g., piriformis syndrome)
3. Why Sciatica Appears to Be Increasing Today
Even though the medical causes are well known, modern life is changing how often they occur or are triggered.
3.1 Prolonged Sitting (The Biggest Driver)
This is the most important modern factor.
People today spend long hours:
- Sitting at desks
- Driving
- Using computers or phones
Long sitting increases pressure on spinal discs and can irritate the lower back nerves over time.
Over time, this can contribute to disc degeneration or worsen existing disc problems.
3.2 Sedentary Lifestyle and Weak Core Muscles
A weak core (abdominal and lower back muscles) means the spine gets less support.
This leads to:
- Poor posture
- Increased spinal load
- Higher risk of disc bulging
Modern lifestyles involve less physical activity than previous generations, increasing vulnerability.
3.3 Obesity and Weight Gain Trends
Extra body weight increases pressure on the spine, especially the lower back. This accelerates disc wear and nerve compression.
3.4 Aging Population
As life expectancy increases, more people are living long enough to develop:
- Disc degeneration
- Arthritis
- Spinal narrowing
These are major sciatica triggers.
3.5 Increased Awareness and Diagnosis
It’s also important to note:
- People are now more aware of sciatica symptoms
- More scans (MRI/CT) are available
- Better reporting leads to more diagnosed cases
So part of the “increase” is better detection, not just more disease.
3.6 Occupational Changes
Modern work often involves:
- Sitting jobs (office work, remote work)
- Long driving hours (ride-hailing, delivery jobs)
- Less physical movement during the day
This combination creates a “perfect storm” for lower back strain.
4. What Actually Happens in the Body?
A simple breakdown:
- Disc weakens (age, posture, pressure)
- It bulges or herniates
- It presses on a nerve root
- The sciatic nerve carries pain signals down the leg
The brain interprets the nerve irritation as leg pain, even though the problem is in the spine.
5. How Sciatica Is Managed and Treated
Most cases do NOT require surgery. Treatment focuses on reducing inflammation, relieving pressure, and strengthening the spine.
5.1 Early Stage Management (First-line care)
Movement (not complete rest)
Light activity helps recovery. Prolonged bed rest often slows healing.
Pain relief options
- Anti-inflammatory medication (as prescribed)
- Heat or cold therapy
Posture correction
- Avoid long sitting without breaks
- Use lumbar support when sitting
5.2 Physiotherapy (Very important)
Physiotherapy focuses on:
- Strengthening core muscles
- Stretching tight hip muscles
- Improving spinal alignment
- Nerve mobility exercises
This is one of the most effective long-term treatments.
5.3 Lifestyle Adjustments
Key changes include:
- Reducing long sitting periods
- Taking frequent walking breaks
- Improving ergonomics at work
- Maintaining healthy body weight
- Regular low-impact exercise (walking, swimming, cycling)
5.4 Medical Interventions (If severe)
If symptoms persist or worsen:
- Steroid injections to reduce inflammation
- Advanced imaging (MRI)
- Surgery (rare, for severe nerve compression or weakness)
6. How to Prevent Sciatica (Long-Term Strategy)
Prevention focuses on protecting the spine daily:
✔ Keep moving
Avoid sitting for long uninterrupted periods.
✔ Strengthen core muscles
Strong core = better spinal support.
✔ Maintain posture awareness
Especially when sitting or lifting.
✔ Stretch regularly
Focus on hips, hamstrings, and lower back.
✔ Manage weight
Reduces pressure on spinal discs.
7. The Big Picture
The rise in sciatica is not due to a single cause—it is a combination of modern lifestyle habits and natural aging processes.
In simple terms:
Our bodies were built for movement, but modern life demands long hours of sitting and low activity.
That mismatch is one of the biggest reasons sciatica is becoming more common.
Sciatica is increasingly common because of:
- Prolonged sitting and sedentary work
- Weak core muscles and poor posture habits
- Aging population and spinal degeneration
- Lifestyle-related weight gain
- Better diagnosis and awareness
The good news is that most cases improve with movement, physiotherapy, and lifestyle correction, without the need for surgery
Never Miss a Story: Join Our Newsletter